Treatment of osteoarthritis
Non-surgical treatment
Physiotherapy

Physiotherapy can be helpful in the early stage of OA. Primary aim of the physiotherapy isto reduce swelling and pain as well train the muscle envelope around the knee joint.
It also might be capable to postpone surgery due to a better muscular protection and proprioception of the knee joint.
Hence, physiotherapy is one of the cornerstones of OA treatment. Healing of OA is however not possible.
Injections

In the early stages of OA or cartilage degeneration an injection of hyaluronic acid and/or glucosamin can result in increased knee quality of life. The course of OA however, can hardly be influenced.
In a later more severe stage of OA, in which the associated chronic synovitis leads to more pain and swelling, it can be helpful to inject the knee with cortison and local anaesthetics. An interval of at least 4-6 weeks between the injections should be followed. A maximum of 3-4 injections can be made.
The risks of infection and osteonecrosis have always to be weighed against the possible clinical benefits.
Insoles, braces
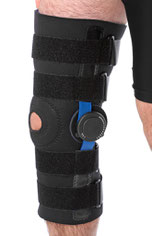
A considerable number of braces, orthotics and bands are available for treatment of OA. In addition, insoles with lateral wedges are proposed for OA treatment. These need to be individually tailored to each patient.
For treatment of a medial compartment OA, in which a varus leg deformity leads to increased stress medially, lateral wedged insoles or braces can be used. However, these are not comfortable and should be consequently worn.
Medication

Pain and anti-inflammatory medication help to reduce pain and inflammation of the knee. These are considered the first treatment to be initiated.
These however, do not change the course of OA over time. To date there is no evidence that any medication is able to positively influence OA. The most commonly used ones are:
- hyaluronic acid
- glucosamin
- others (e.g. teufelskralle, Muschel-Lipp extract)
Surgical treatment
Arthroscopy
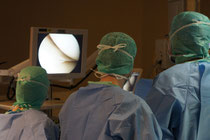
Treatment of OA with arthroscopic debridement is still a matter of debate.
It can be clinically helpful in some exceptional cases, in which a joint replacement should be performed.
In particular, a blocked knee due to degenerative meniscal lesions is a good indication to perform an arthroscopy in OA.
Correction osteotomy of leg axis
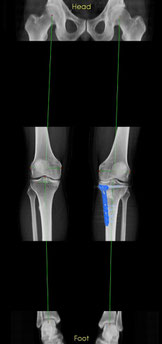
A varus (bowed shaped leg) or valgus (x-shaped leg) can lead to chronic overloading of the medial or lateral knee compartment and finally to OA.
A correction osteotomy is able to change the leg alignment from a varus into a valgus knee, which then leads to decreased joint loading. In best sense it is able to slow down or prevent OA of the knee.
Here you find an image of a right and left knee. On the left there is a knee with a varus alignment and on the right a knee after correction osteotomy. The plate is shown in blue.
Partial knee replacement

A partial knee replacement is indicated when only a single knee compartment is affected by OA (medial tibiofemoral, lateral tibiofemoral, patellofemoral).
In such a case a selective resurfacing of the affected knee compartment should be performed. The surface of the knee compartment is replaced by metal and plastic.
For OA of the tibiofemoral joint (medial or lateral) a unicondylar knee replacement and for OA of the patellofemoral joint a patellofemoral joint replacement can be performed.
In the picture you find an example of an unicondylar knee replacement.

Here you see a partial knee replacement, named patellofemoral joint replacement. It addresses a patellofemoral OA.
The femoral trochlea is replaced with a metal component and the patellar joint surface by a polyethylene part.
Total knee replacement

In contrast to a partial knee replacement a total knee replacement resurfaces all knee compartments (medial tibiofemoral, lateral tibiofemoral, patellofemoral).
A total knee replacement is indicated, when all joint compartments are affected by OA. OA can be identified on radiographs. In these typically a sclerosis, narrowed joint gaps, cysts and osteophytes are present.
Not only the radiographs determine the final treatment. Moreover, it is a combination of your symptoms (pain, limited range of motion, stiffness), radiographs, clinical examination and undergone non-surgical treatment options.
Caveat: Never undergo a partial or total knee replacement, when you do not experience any knee pain!

 Ihr Kniespezialist in Basel
www.kniedoktor.ch
Your English speaking Chirurgie du genou specialise
knee expert in Basel! expert a Bale
www.kneesurgeon.ch www.kneedoctor.ch
Ihr Kniespezialist in Basel
www.kniedoktor.ch
Your English speaking Chirurgie du genou specialise
knee expert in Basel! expert a Bale
www.kneesurgeon.ch www.kneedoctor.ch